
Introduction
When a senior is living with cancer, heart failure, advanced dementia, kidney disease, or another serious diagnosis, movement begins to look very different than it did a year or two earlier. Walking the dog or carrying groceries gives way to slower, more measured efforts: a short walk to the kitchen, a careful transfer from bed to chair, a few minutes seated by the window. Mobility support for seniors with advanced illness is not about pushing for rehabilitation gains. It is about preserving comfort, safety, and the kind of small, daily movement that protects dignity and quality of life.
Families often feel caught between two instincts. One says, “Keep them moving so they don’t decline.” The other says, “Don’t push, they’re exhausted.” Both impulses come from love, but neither is a plan. The right approach lies somewhere in the middle, and it shifts week to week as the illness progresses. The goal is no longer recovery in the traditional sense. The goal is to make every transfer, every step, and every position change as safe and as comfortable as it can be.
This guide is written for the spouse, adult child, or family caregiver who is trying to do right by someone they love. It explains how mobility goals change during advanced illness, what equipment and techniques actually help, where things commonly go wrong, and how to recognize when it is time to step back from active mobility and focus entirely on comfort. You do not need to be a nurse or therapist to read it. You only need to want to understand.
Why Advanced Illness Changes the Mobility Picture
In healthy aging, the conversation around movement usually centers on prevention. We focus on strength training, balance work, and fall reduction in order to extend independence. When a senior enters the advanced stages of a serious illness, that framework no longer fits cleanly. The body is dealing with disease processes that reduce energy, change muscle composition, and often introduce new symptoms like pain, breathlessness, or confusion. Asking someone in this stage to “exercise more” can be both unrealistic and unkind.
Palliative care medicine offers a more useful lens. According to Get Palliative Care, palliative care is specialized medical care for people living with a serious illness, focused on relieving symptoms and improving quality of life. Within that framework, mobility support for seniors with advanced illness becomes one piece of a larger comfort plan. Movement is preserved not for its own sake but because it serves the person: a few steps to the bathroom protects dignity, a transfer to a recliner reduces pressure injuries, a careful repositioning in bed eases pain.
This reframing matters because it changes what success looks like. Success is no longer measured in walking distance or rehabilitation milestones. It is measured in whether the senior could shift positions without pain, whether they got to the chair by the window today, whether the family could help them safely without anyone getting hurt. Families who understand this shift early often feel less guilt and more clarity. If you are still adjusting to the change in pace, our companion guide on how to support a loved one with limited mobility walks through the emotional and practical groundwork in more detail.
The Three Pillars of Comfort-Focused Mobility
Healthcare teams who specialize in advanced illness tend to organize mobility around three connected goals. Thinking of them as pillars helps families decide where to put their energy and which tradeoffs are worth making.
The first pillar is comfort. Every movement should be as painless as possible. That means slowing the pace, timing transfers around pain medication doses, padding hard surfaces, and respecting the senior’s signals. If a particular position causes pain, find another one. Comfort is not a soft goal during advanced illness — it is the foundation on which everything else rests.
The second pillar is safety. Falls, skin tears, and caregiver injuries become more likely as a senior weakens. Mobility support for seniors with advanced illness has to account for both the senior’s safety and the caregiver’s. A transfer that hurts the caregiver’s back today means a less capable caregiver next week. Safety planning includes the right equipment, enough help, and a willingness to stop a transfer if something feels wrong.
The third pillar is dignity. Many seniors in advanced illness lose access to private activities they once took for granted: walking to the bathroom, dressing themselves, sitting at the dinner table. Preserving these moments where possible — or finding gentle, respectful alternatives when they are no longer possible — matters as much as any medical intervention. Dignity is what tells a senior they are still themselves, even when their body is changing.

What Goes Wrong Without a Plan
Families who try to manage advanced illness mobility without a clear plan often run into the same handful of problems. The first is a slow drift into avoidance. Each transfer becomes a little harder, so the family stops attempting them. The senior spends more and more hours in the same chair or the same position in bed. Within weeks, deconditioning sets in, pressure injuries develop, and a senior who could have managed a daily move to the recliner becomes someone who cannot safely move at all.
The second common failure point is caregiver injury. A spouse or adult child tries to lift a frail senior without equipment or training, twists their back, and is suddenly unable to provide care at all. The CDC notes that falls are the leading cause of injury among older adults, but caregiver injuries also rise sharply when transfers happen without proper technique or support. One bad transfer can sideline a primary caregiver for weeks.
A third failure pattern is fall avoidance taken too far. Out of fear, the family confines the senior to bed even when sitting up or moving to a recliner would have been safe with the right support. Total bed rest, when it isn’t medically required, accelerates muscle loss, increases pressure injury risk, and worsens mood. Good mobility support for seniors with advanced illness is not about more activity or less activity. It is about the right kind of activity at the right time, with the right help.
A fourth, quieter failure is the lack of communication with the medical team. The hospice nurse or palliative care doctor cannot adjust the plan if they don’t know the senior is now skipping bathroom trips because of pain, or that the caregiver is afraid to attempt transfers. Calling these issues out early lets the team respond with medication adjustments, additional equipment, or extra in-home help.
Repositioning and Bed-Based Mobility
For many seniors in advanced stages of illness, most of the day will be spent in bed or in a recliner. Repositioning becomes the most important form of movement. Done well, it prevents pressure ulcers, eases breathing, reduces stiffness, and keeps the senior comfortable without requiring full transfers.
A simple repositioning rhythm works for most situations: every two hours during the day, the senior should shift to a new position. That can mean turning slightly to one side, propping up with pillows, raising the head of an adjustable bed, or coming up to sit on the edge for a few minutes if it is tolerated. The goal is not a full workout. It is to break up pressure on any one part of the body and give the lungs, joints, and skin a different angle to work with. Our guide on how to prevent pressure ulcers covers the specific positioning techniques in depth and is a useful companion to this section.
Equipment makes a real difference here. An adjustable bed with a remote control allows the head and feet to move without anyone having to lift the senior manually. A pressure-relieving mattress overlay distributes weight more evenly. Slide sheets, used under the hips and shoulders, let a caregiver reposition the senior without dragging skin across the bedding. A small wedge pillow under one hip relieves pressure on the lower back. None of this equipment is expensive compared to a hospital readmission for a pressure injury, and most of it can be obtained through hospice services if the senior is enrolled.
Caregivers should also pay attention to their own body mechanics during repositioning. Keep the bed at hip height when possible. Stand close to the senior, not at arm’s length. Use your legs, not your back, to shift weight. If you feel yourself straining, stop and ask for help. There is no version of this work where the caregiver’s own health is optional.
Transfers, Walkers, and Wheelchairs in Advanced Illness
Even in advanced stages, many seniors can still manage some level of transfer with the right setup. The right tools matter more than ever because the margin for error is small. Mobility support for seniors with advanced illness during transfers focuses on three questions: Is this transfer worth the energy cost? Is it safe for both people? Is there a piece of equipment that would make it easier?
A rolling walker with a padded seat is often the most useful daily aid. It supports the senior on short walks to the bathroom or dining area and offers an immediate place to sit if fatigue hits. For seniors who cannot manage walking, a transport wheelchair allows family members to move them comfortably between rooms or out into a sunny patio without requiring the senior to bear weight. A bedside commode positioned beside the bed eliminates the need for a longer walk to the bathroom and is often the single most useful piece of equipment in the final months of an illness.
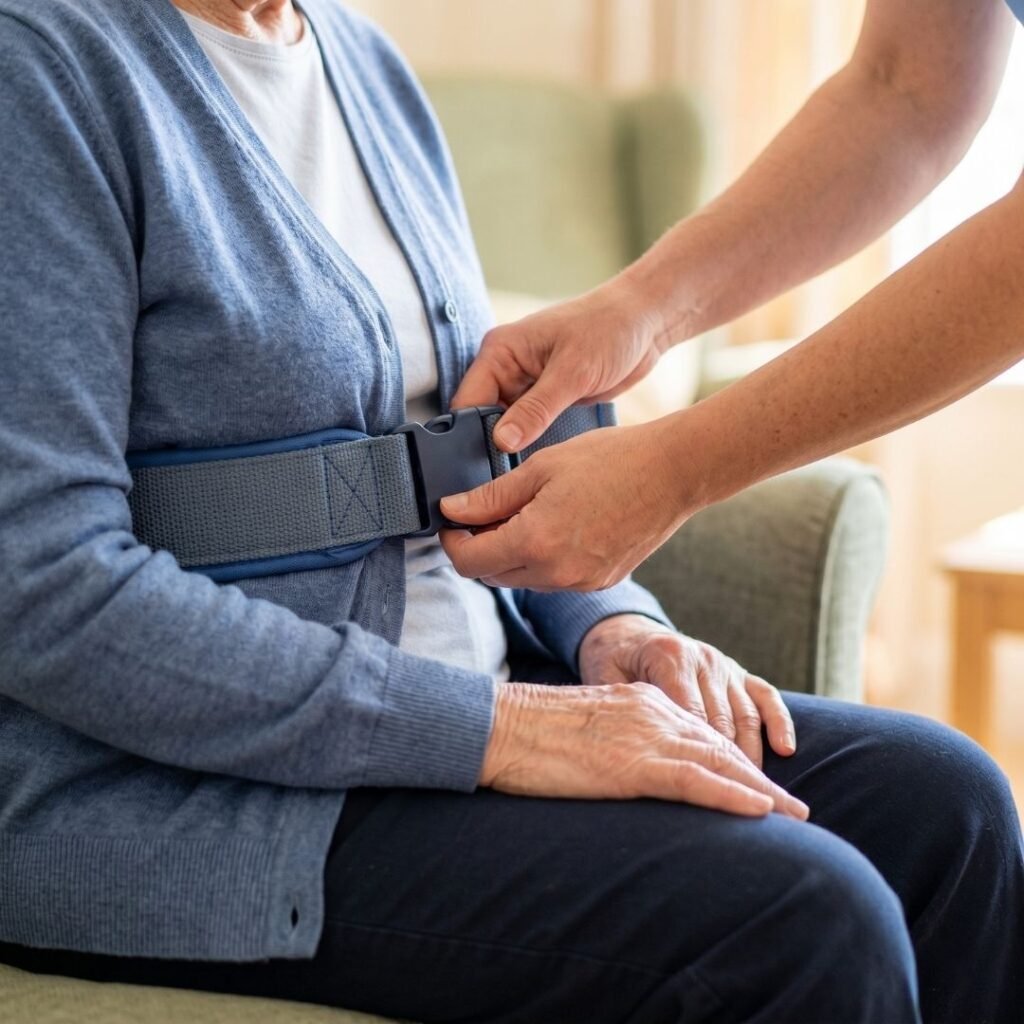
For sit-to-stand transfers, a padded gait belt fitted around the senior’s waist gives the caregiver a secure place to grip without pulling on the senior’s arms or clothing. A floor-to-ceiling transfer pole near the bed or recliner gives the senior something stable to hold while they rise or pivot. When the senior can no longer assist with transfers at all, a hospice or palliative care team can often arrange a sit-to-stand lift or a full sling lift for the home. Families sometimes resist this equipment because it feels like a step backward, but a mechanical lift used kindly is far more dignified than a fall.
Comfort Positioning and Out-of-Bed Time
Even when full mobility is no longer possible, time out of bed remains valuable for as long as it is comfortable. A senior who can spend an hour or two in a padded recliner, with a footrest raised and a soft blanket, often experiences less stiffness, better appetite, and more meaningful interaction with the family. That hour is not measured in steps. It is measured in quality of life.
Setting up a comfort chair zone is one of the most useful things a family can do. Choose a recliner that allows for both leaning back and lifting the feet, and place it where the senior wants to be — near the window, close to a grandchild’s play area, in front of a favorite view. Keep a small table within reach with water, tissues, lip balm, hand cream, a phone, and any items that bring comfort. A footstool, an extra cushion behind the lower back, and a soft blanket cover most needs. The point is to make the chair its own destination, not just a midpoint between bed and bathroom.
For seniors who can no longer transfer to a chair, comfort positioning in bed becomes the priority. A wedge pillow that lifts the upper body can ease breathing. Pillows tucked under the knees relieve lower back tension. A small rolled towel behind one shoulder shifts pressure away from a sensitive area. None of these adjustments require special equipment, and the cumulative effect on comfort can be significant. Encourage the senior to tell you what feels better and what does not. Their feedback is the most reliable guide you have.
Special Considerations: Pain, Breathlessness, and Cognitive Change
Three symptoms shape mobility decisions more than any others during advanced illness: pain, breathlessness, and cognitive change. Each one calls for a slightly different approach.
When pain is the main issue, mobility should be timed around pain medication. If a dose is given thirty to forty-five minutes before a planned transfer, the senior will tolerate the movement far better. Avoid surprise transfers. Tell the senior what you are about to do, give them a moment, and move slowly. Painful joints often benefit from warm compresses before a transfer, and pillows placed strategically can take pressure off the most tender areas.

When breathlessness dominates, the senior often cannot lie flat. Mobility shifts toward upright positions: a raised hospital bed, a recliner, or pillows propped at a steep angle. Short distances are tolerated better than long ones, and any walk should pause for rest before the senior asks. A bedside commode often replaces walks to the bathroom because the energy cost of a longer trip becomes too high.
When cognitive change — including delirium, dementia, or end-stage confusion — is part of the picture, the senior may resist transfers, forget the steps, or move unsafely without warning. In these cases, mobility support for seniors with advanced illness leans heavily on routine and predictability. Use the same simple words for each transfer. Approach from the same side. Keep the environment uncluttered so there are fewer visual surprises. And accept that some days the senior will simply not be able to participate, and that is not a failure of caregiving.
Throughout all three of these patterns, stay in close contact with the palliative care or hospice team. They can adjust medications, order additional equipment, and offer hands-on coaching. Many families also benefit from talking to others walking the same path, and our guide on coping with reduced mobility offers grounding for the emotional side of this work.
Frequently Asked Questions
1. How do mobility goals change for a senior with an advanced illness?
Mobility goals shift away from rehabilitation and toward comfort, safety, and dignity. Instead of measuring progress in walking distance or strength gains, families and care teams focus on whether the senior can shift positions without pain, transfer to a favorite chair, or reach the bathroom safely. Daily movement still matters, but its purpose is to preserve quality of life rather than to prevent decline.
2. Should a senior with advanced illness still get out of bed every day?
In most cases, yes — for as long as it is comfortable. Time out of bed protects skin, lungs, joints, and mood, and even a short period in a recliner can make a meaningful difference. The exception is when getting up causes pain that cannot be controlled, when the senior is too weak to participate at all, or when the medical team has advised otherwise. Mobility support for seniors with advanced illness adapts to the day, not the calendar.
3. What mobility aids are most useful in palliative or hospice care at home?
The most useful pieces of equipment are usually an adjustable bed, a pressure-relieving mattress, a bedside commode, a rolling walker with a seat, a transport wheelchair, a padded gait belt, and slide sheets for repositioning. As the illness progresses, a sit-to-stand lift or a full sling lift may also become important. Hospice agencies often provide most of this equipment at no extra cost to the family.
4. How can family caregivers move a frail senior without causing pain?
Time transfers around pain medication doses, move slowly, and explain each step before doing it. Use a padded gait belt rather than pulling on arms or clothing. Keep your own body close to the senior and use your legs, not your back. Pad any hard surfaces the senior will rest against, and stop immediately if the senior signals pain. When in doubt, ask the hospice or palliative care team to demonstrate a safer technique in person.
5. When is it time to stop pushing for active mobility and focus on comfort?
There is usually no single moment, but several signs point in that direction: transfers consistently cause pain, the senior is sleeping most of the day, they no longer want to get out of bed, or attempts at movement leave them exhausted for hours. At that stage, mobility support for seniors with advanced illness usually narrows to gentle repositioning in bed, careful skin care, and presence. The work is no longer about movement at all. It is about being there.
Final Thoughts
Caring for a senior with an advanced illness asks more of a family than almost any other stage of life. The work is physically demanding, emotionally heavy, and rarely seen by anyone outside the home. Mobility support for seniors with advanced illness is one of the most concrete ways that love shows up: in the careful transfer to a recliner, the soft pillow tucked behind a tired shoulder, the quiet decision to pause when a transfer no longer feels right.
The most important thing to remember is that there is no perfect plan. The illness will keep changing, and the right approach next month will look different from the right approach today. Families who do this work well are not the ones who get every move right. They are the ones who stay attentive, ask for help, lean on their palliative care or hospice team, and adjust the plan as the situation evolves.
If you are in the middle of this season, give yourself credit for the daily decisions that no one else sees. You are not failing your loved one by slowing down, by using equipment, or by accepting that some mornings the goal is only to make them comfortable. You are providing exactly the kind of care that this stage of life requires. Mobility support for seniors with advanced illness is, in the end, an act of love translated into small, practical choices — one transfer, one position change, one quiet hour by the window at a time.
Medical Disclaimer: The information provided on this website is for educational purposes only and should not replace professional medical advice. Always consult your physician or qualified healthcare provider regarding any medical condition or treatment decisions.

